ACLS Exam Version A and B Combined_Advanced Cardiovascular Life Support. 100 Q&A
- PDF
Description
ACLS Exam Version A and B Combined_Advanced Cardiovascular Life Support. 100 Q&A
Advanced Cardiovascular Life Support Exam Version A (50 questions)
Please do not mark on this exam. Record the best answer on the separate answer sheet.
1. You find an unresponsive patient who is not breathing. After
activating the emergency response system, you determine that
there is no pulse. What is your next action?
A. Open the airway with a head tilt–chin lift.
B. Administer epinephrine at a dose of 1 mg/kg.
C. Deliver 2 rescue breaths each over 1 second.
D. Start chest compressions at a rate of at least 100/min.
2. You are evaluating a 58-year-old man with chest pain. The blood
pressure is 92/50 mm Hg, the heart rate is 92/min, the nonlabored
respiratory rate is 14 breaths/min, and the pulse oximetry reading
is 97%. What assessment step is most important now?
A. PETCO2
B. Chest x-ray
C. Laboratory testing
D. Obtaining a 12-lead ECG
3. What is the preferred method of access for epinephrine
administration during cardiac arrest in most patients?
A. Intraosseous
B. Endotracheal
C. Central intravenous
D. Peripheral intravenous
4. An activated AED does not promptly analyze the rhythm. What is your
next action?
A. Begin chest compressions.
B. Discontinue the resuscitation attempt.
C. Check all AED connections and reanalyze.
D. Rotate AED electrodes to an alternate position.
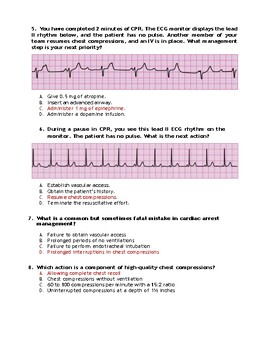
5. You have completed 2 minutes of CPR. The ECG monitor displays the lead
II rhythm below, and the patient has no pulse. Another member of your
team resumes chest compressions, and an IV is in place. What management
step is your next priority?
A. Give 0.5 mg of atropine.
B. Insert an advanced airway.
C. Administer 1 mg of epinephrine.
D. Administer a dopamine infusion.
6. During a pause in CPR, you see this lead II ECG rhythm on the
monitor. The patient has no pulse. What is the next action?
A. Establish vascular access.
B. Obtain the patient’s history.
C. Resume chest compressions.
D. Terminate the resuscitative effort.
7. What is a common but sometimes fatal mistake in cardiac arrest
management?
A. Failure to obtain vascular access
B. Prolonged periods of no ventilations
C. Failure to perform endotracheal intubation
D. Prolonged interruptions in chest compressions
8. Which action is a component of high-quality chest compressions?
A. Allowing complete chest recoil
B. Chest compressions without ventilation
C. 60 to 100 compressions per minute with a 15:2 ratio
D. Uninterrupted compressions at a depth of 1½ inches
9. Which action increases the chance of successful conversion of
ventricular fibrillation?
A. Pausing chest compressions immediately after a defibrillation attempt
B. Administering 4 quick ventilations immediately before a defibrillation attempt
C. Using manual defibrillator paddles with light pressure against the chest
D. Providing quality compressions immediately before a defibrillation attempt
10. Which situation BEST describes pulseless electrical activity?
A. Asystole without a pulse
B. Sinus rhythm without a pulse
C. Torsades de pointes with a pulse
D. Ventricular tachycardia with a pulse
Advanced Cardiovascular Life Support Exam Version B (50 questions)
Please do not mark on this exam. Record the best answer on the separate answer sheet.
1. What should be done to minimize interruptions in chest compressions during CPR?
A. Perform pulse checks only after defibrillation.
B. Continue CPR while the defibrillator is charging.
C. Administer IV medications only when breaths are given.
D. Continue to use AED even after the arrival of a manual defibrillator.
2. Which condition is an indication to stop or withhold resuscitative efforts?
A. Unwitnessed arrest
B. Safety threat to providers
C. Patient age greater than 85 years
D. No return of spontaneous circulation after 10 minutes of CPR
3. After verifying the absence of a pulse, you initiate CPR with adequate bag-mask
ventilation. The patient’s lead II ECG appears below. What is your next action?
A. IV or IO access
B. Endotracheal tube placement
C. Consultation with cardiology for possible PCI
D. Application of a transcutaneous pacemaker
4. After verifying unresponsiveness and abnormal breathing, you activate
the emergency response team. What is your next action?
A. Retrieve an AED.
B. Check for a pulse.
C. Deliver 2 rescue breaths.
D. Administer a precordial thump.
5. What is the recommendation on the use of cricoid pressure to prevent aspiration
during cardiac arrest?
A. Not recommended for routine use
B. Recommended during every resuscitation attempt
C. Recommended when the patient is vomiting
D. Recommended only for supraglottic airway insertion
6. What survival advantages does CPR provide to a patient in ventricular fibrillation?
A. Increases the defibrillation threshold
B. Directly restores an organized rhythm
C. Opposes the harmful effects of epinephrine
D. Produces a small amount of blood flow to the heart
7. What is the recommended compression rate for performing CPR?
A. 60 to 80 per minute
B. 80 to 100 per minute
C. About 100 per minute
D. At least 100 per minute
8. EMS personnel arrive to find a patient in cardiac arrest. Bystanders are performing
CPR. After attaching a cardiac monitor, the responder observes the following
rhythm strip. What is the most important early intervention?
A. Defibrillation
B. Endotracheal intubation
C. Epinephrine administration
D. Antiarrhythmic administration
9. A patient remains in ventricular fibrillation despite 1 shock and 2 minutes of
continuous CPR. The next intervention is to
A. administer amiodarone.
B. administer a second shock.
C. administer epinephrine.
D. insert an advanced airway.
10. What is the recommended next step after a defibrillation attempt?
A. Open the patient’s airway.
B. Determine if a carotid pulse is present.
C. Check the ECG for evidence of a rhythm.
D. Begin CPR, starting with chest compressions.
(PURCHASE TO ACCESS ALL 100 Q&A)